2025 NYC Heat-Related Mortality Report
Each summer, on average, more than 500 New Yorkers die prematurely because of hot weather in New York City. In the most recent five-year period (2018-2022), an estimated 525 people died annually due to heat. These heat-related deaths account for about 3% of all deaths over the warm season months of May through September. Of the 525 deaths:
- There was an average of 5 heat-stress deaths (caused directly by heat) per year.
- There was an average of about 520 heat-exacerbated deaths (caused indirectly by heat aggravating an underlying illness) per year.
Heat-exacerbated deaths increased in the past decade, mainly due to hotter summers overall with more “non-extreme hot days” of 82°F up to but below the extreme heat threshold (95°F). Estimates of the number of deaths have remained relatively steady in the most recent years. The 2018-2022 estimate is similar in magnitude to the 2017-2021 estimate of 570 in last year’s report, with more than 500 New Yorkers dying due to the heat every summer. The number of heat-exacerbated deaths in last year’s report was corrected to 570. See details on the correction here.
Black New Yorkers are more likely to die from heat stress, with death rates two times higher than white New Yorkers. Black New Yorkers also have a higher likelihood of heat-exacerbated death compared to other New Yorkers. This inequity is due to past and current structural racism that creates economic, health care, housing, energy, and other systems that benefit white people and disadvantage people of color.
Lack of access to home air conditioning (AC) is the most important risk factor for heat-stress death. Among those who died from heat stress, the place of death was most often an un-air-conditioned home. Heat-exacerbated deaths were also more likely to occur at home, underscoring the importance of access to cooling at home.
NYC summers are getting hotter because of climate change. Emergency response to extreme heat must be coupled with equitable investments in structural interventions and heat mitigation measures that reduce risk throughout the season. For example, all New Yorkers will need energy-efficient home cooling that they can afford to run; tree planting and greening can help reduce local temperatures while providing shade.
Introduction
Hot weather is dangerous to health, sometimes resulting in death. Heat-related deaths are preventable. In this fifth annual report on heat-related mortality, the NYC Health Department reports on heat-related deaths in three ways:
- Heat-stress deaths (also called heat stroke deaths) are caused directly by heat and happen when heat-related illnesses, such as heat exhaustion and hyperthermia, lead to death. These deaths are coded as heat-related in death certificates, and cases can be counted and investigated.
- Heat-exacerbated deaths happen when heat worsens existing chronic conditions, such as heart disease. These deaths are caused indirectly by heat and are estimated using statistical models. They are also often called “excess” mortality.
- Neighborhood impacts are tracked by looking at community-level differences in risk of heat-related death and are described using the NYC Health Department’s Heat Vulnerability Index (HVI).
We report estimated trends in heat-exacerbated deaths for the current and past several decades (1973-2022) in five-year rolling time windows. For heat-stress deaths, we report counts and the annual average for the past ten years (2014-2023). Please refer to the footnote on years of data available for more information about the years of data included in this report. Read reports from previous years.
Heat Stress Deaths
The NYC Health Department examined heat-stress deaths occurring during the warm season months of May through September from 2014-2023. We reviewed death certificates and medical examiner investigation reports in cases where heat was recognized as a cause of death. A more detailed description of methods and data sources can be found in the Appendix Methods and Supplemental Data.
Among NYC residents, there were 49 heat-stress deaths over the 10-year period, which included one year (2014) with no extreme heat events (Figure 1). There was an average of 5 deaths per year. Most deaths occurred in July (61%), followed by August (16%), June (8%), September (8%), and May (6%). As of January 2025, there were 3 heat-stress deaths in 2024, though that number is provisional and subject to change because mortality records are not yet finalized.
Demographics
- Black New Yorkers continue to have an age-adjusted heat-stress death rate that is twice as high as that of white New Yorkers (0.8 deaths per million compared with 0.4 deaths per million) from 2014-2023. This inequity is rooted in systemic racism [1]. Lack of equitable access to resources — for example, jobs that pay a living wage, affordable and healthy housing with air conditioning, and health care — are causes of these differences in heat-related mortality.
- Death rates were higher in neighborhoods with more than 30% of residents having a household income below the federal poverty line compared with wealthier neighborhoods.
- Heat-stress deaths occurred among all age groups, with the lowest rates among people ages 20 and younger and the highest among people ages 60 and older.
- Rates of heat-stress deaths were higher among males than females.
- Age-adjusted death rates were highest in Brooklyn and Queens.
Figure 2: Demographic characteristics of heat-stress decedents (2014-2023).
Health Risk Factors
Among decedents with detailed medical examiner records available, 89% had at least one chronic health condition.
Common conditions included cardiovascular disease, substance or alcohol use, mental health or cognitive conditions, lung conditions, and a history of diabetes.
Table 1: Medical characteristics among subset with review of health conditions in medical examiner records (n=46) (2014-2023).
Heat Exposure Circumstances
People who died from heat stress were most often exposed to dangerous heat in homes (45%, n=20 of 44 records with detailed information available about onset place). Among New Yorkers exposed in homes, and for whom there was information about the presence or absence of an AC (n=15), none had or were using AC. Without AC, indoor temperatures can be much higher than outdoors, especially at night, and can continue for days after a heat wave [2].
Of people exposed to dangerous heat at home, about a quarter (n=5, 25%) had an electric fan present and on, indicating that using an electric fan without an AC cannot always prevent death during extreme heat for people who are at highest heat risk.
Air conditioning access differs across race and class. Black New Yorkers and low-income New Yorkers are less likely to own or use an AC during hot weather because of the cost [3]. In addition, access varies by neighborhood. About 90% of NYC households currently have air conditioning, but access can be much lower in neighborhoods where more people are living with limited financial resources.
The next most common place of heat exposure was outdoors (n=19, 43%). Another 7% (n=3) were exposed in parked cars, 2% (n=1) were exposed indoors at a worksite, 2% (n=1) were exposed on a subway platform.
Overall, 11% (n=5) of deaths were work-related and another 14% (n=6) were individuals noted to be experiencing or suspected to be experiencing homelessness.
Table 2: Air conditioning presence among heat-stress decedents exposed to heat in homes (2014-2023).
Heat Exacerbated Deaths
Deaths from chronic conditions that are not recognized as heat-related on death certificates can be estimated using statistical models. There are many more of these deaths than those from heat stress. They are called “excess deaths” or “heat-exacerbated deaths.” Unlike heat-stress deaths, which can be individually identified and investigated, excess deaths can be estimated only as aggregate counts. However, estimating heat-exacerbated deaths — or “mortality” — better captures the true extent of how many New Yorkers are dying due to heat.
We report estimated heat-exacerbated deaths for the current and historical data in five-year rolling time windows to characterize trends. In the summary, we round point estimates to the nearest 10, to avoid conveying a false sense of precision about modeled estimates. The average natural death count per year was about 19,000 for May through September for the most recent 5-year period (2018-2022). We used time-series statistical models to compare deaths on hot days with those on cooler days. We estimated heat-exacerbated deaths using:
- An indicator (yes/no) for extreme heat event days defined by the National Weather Service’s heat advisory levels for NYC. Based on the NYC Health Department’s previous analysis of heat-exacerbated mortality, heat advisories are for at least two consecutive days with 95°F or higher daily maximum heat index (HI) or any day with a maximum HI of 100°F or higher.
- A range of hot daily maximum temperatures that includes both extreme heat event days and other hot days. We estimated heat-exacerbated deaths for days ranging from the median maximum daily temperature of 82°F through the highest temperature during the period.
These models were run in five-year rolling time windows between 1973 and 2022 (last year’s report included 1972 to 2021). We included deaths occurring on the date of exposure to hot weather and over the following three days because previous NYC Health Department studies have shown that heat-exacerbated deaths can occur up to three days after the initial hot weather [4]. Detailed methods used to estimate risks and attributable deaths can be found in the Appendix Methods and Supplemental Data.
Estimated heat-exacerbated deaths — both those attributed to extreme and non-extreme hot days — declined substantially between 1972 and 2000 and plateaued after 2000 for about a decade. Heat-exacerbated deaths at and above 82°F then started increasing about a decade ago but plateaued again in recent years (see Figure 3).
From 2018 to 2022, the most recent five-year time window, the estimated annual average of heat-exacerbated deaths during May-September for all hot days was 516 (95% Confidence Interval [95% CI]: 146, 868). Heat-exacerbated deaths made up approximately 3% of all natural-cause deaths in the warm months in this most recent period. Given the wide confidence intervals, this estimate is similar in magnitude to last year’s estimate of 570. (The number of heat-exacerbated deaths in last year’s report was corrected to 570).
The estimated annual average of heat-exacerbated deaths due to extreme heat events for 2018-2022 was 109 (95% CI: 43, 170) — approximately 20% of heat-related deaths. In contrast to the trend for both extreme and non-extreme hot days, heat-exacerbated deaths due to only extreme heat days are relatively constant over the past decade (see Figure 3).
Heat-exacerbated mortality risks were observed across the full range of hot days (maximum temperature at or above 82°F) during warm season months. Risk increased with temperature, with the largest increases occurring at the highest temperatures, and a steeper slope of relative risk above 90°F (see Figure 4). Note that, because there are more days in the range of non-extreme hot days (i.e., 82-94°F) than those in the extreme heat days (95+°F; see the histogram below the relative risk curve), these non-extreme hot days contribute more to the total heat-exacerbated deaths than the days in the extreme heat range.
Figure 3: Annual average heat-exacerbated deaths for Extreme Heat Event days, and days at or above 82°F in five-year moving time windows.
Figure 4: cumulative relative risk and 95% confidence intervals of heat-exacerbated deaths for daily maximum temperature over same-day and three previous days, May-September (2013-2022). 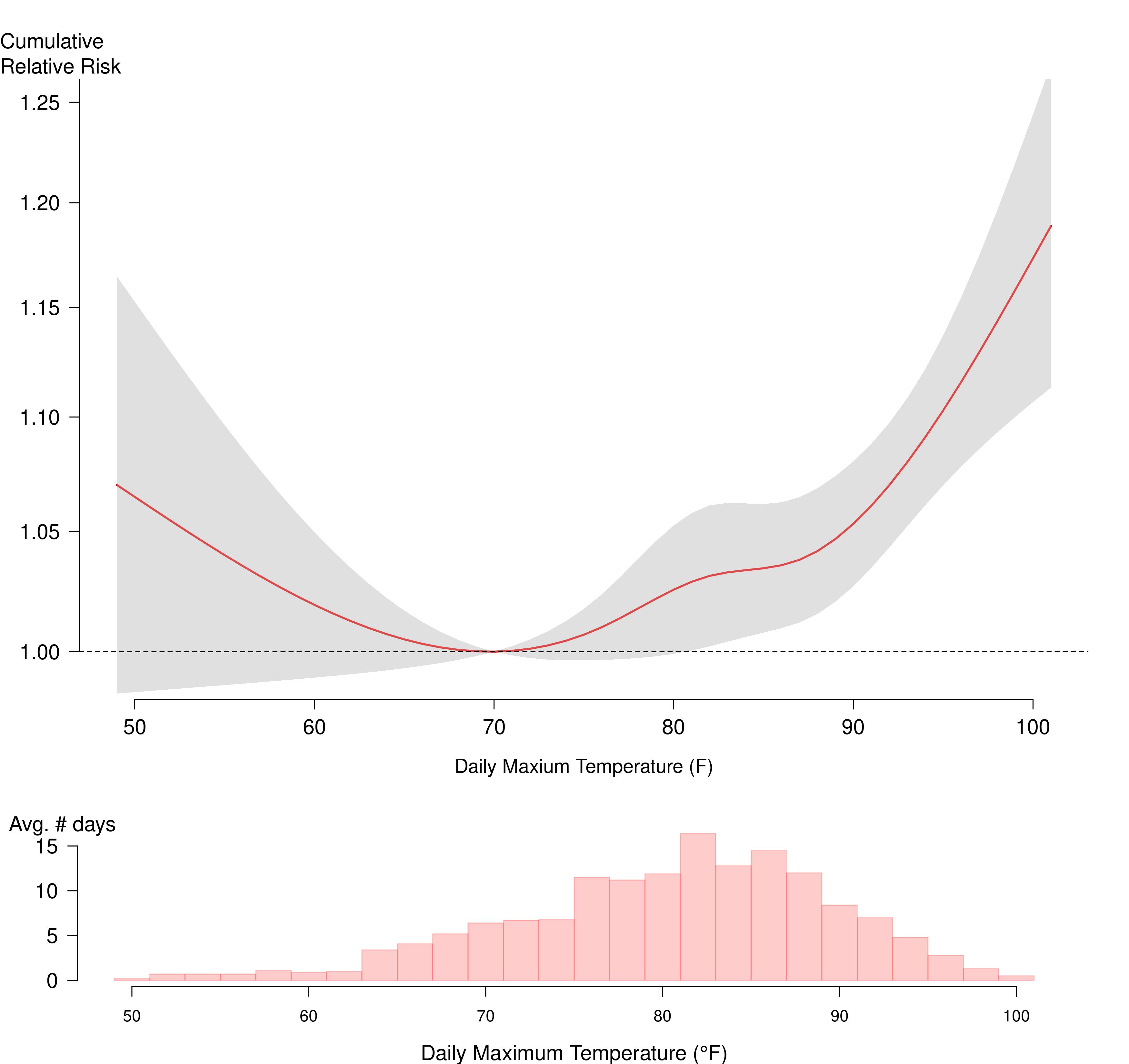
Risk Factors Associated With Heat-Exacerbated Deaths
Our updated analyses of heat-exacerbated deaths confirmed the continued elevated risk of dying at home, as well as higher odds of death among Black New Yorkers compared with other groups.
In previous analyses, heat-exacerbated deaths occurring at home increased during and shortly after extreme heat events (i.e., at or above the NYC heat advisory threshold), and Black New Yorkers had higher odds of death compared to other New Yorkers during the years 2000-2011 [5]. We repeated this case-only analysis with recent data (May – September 2013-2022). We also examined at-home deaths (approximately 28 percent of all deaths during the study period) to see how the proportion of at-home deaths changes by temperature across the entire warm season temperature range. For this analysis, we used five temperature ranges (quintiles of the average of the same day through the previous three days daily maximum temperature). See the Appendix Methods and Supplemental Data for more information.
Similar to previous analyses, we found elevated risk of death for Black New Yorkers. The odds of death for Black New Yorkers on extreme heat days during 2013-2022 was 1.06 (95% CI: 1.02, 1.11). There is also elevated risk of death at home. The overall odds ratio for at-home deaths during 2013-2022 was 1.05 (95% CI: 1.01, 1.10). Figure 5 shows the odds ratios of the at-home deaths as a function of the five temperature ranges with days less than 74°F as the reference. Although the odds ratio — the proportion of at-home deaths relative to that for days with daily maximum temperature less than 74°F — was highest for the hottest temperature range (>86°F), the other temperature ranges also show elevated odds of dying at home. This suggests that the risk of dying at home increases as the temperature increases - both at hot and extreme temperatures.
At-home risk was elevated across racial and ethnic groups, further underscoring the importance of at-home cooling, irrespective of race and ethnicity. The proportion of at-home deaths for non-Hispanic white, Black, and Hispanic New Yorkers were highest at the hottest temperatures (Figure 6). The number of deaths for Asian decedents — about nine percent of all deaths — and decedents of other race and ethnicities were too small to estimate results with precision.
Figure 5: Odds ratios (relative to < 74°F range) and 95% confidence bands of at-home deaths as a function of range (quintiles) of daily maximum temperature averaged over the date of death and three previous days.
Hotter summers
The five average temperature range categories (of 0-3 days average of daily maximum temperature) used in the analysis above each account for approximately 20% of days (i.e., quintiles) in the warm months (May through September) during 2013-2022. Due to climate change, the proportion of the number of days in the higher temperature ranges have been increasing. Figure 7 shows the average number of days over running 10-year time windows for each of the five temperature ranges since 1973.
- The number of days in the two hotter temperature ranges (84-86°F and >86°F) have been increasing, while the number of days in the two cooler temperature ranges (<74°F and 74-79°F) have been declining. In particular, the hottest temperature range (>86°F) had the fastest increase, with the number of days >86°F more than doubling from an average of 14 to 32 days per summer over the five decades, with a steadily increasing trend.
- The measurable and significant rise in hot summer days highlights the urgency for the city to achieve universal access to at-home cooling, combined with equitable access to affordable energy for low-income households to ensure safe indoor thermal environments for the even hotter summers anticipated in the coming decades.
- Occupational heat safety standards for outdoor temperature are also needed to ensure safe working conditions for outdoor workers.
Figure 7: Trend in the number of days per warm season (May-September, 153 days) for the 4-day average daily maximum temperature across five temperature ranges.
Community-Level Impacts
The Heat Vulnerability Index (HVI) shows differences in community-level heat impacts during and shortly after extreme heat events [5]. The HVI combines environmental factors (measures of a neighborhood’s average surface temperature and percentage of green space) with social factors (percentage of homes with air conditioning, residents’ median income, and the percentage of residents who are Black) to develop a relative measure of a neighborhood vulnerability to heat.
Unlike many social vulnerability indices, the HVI is derived from NYC mortality data, which means that neighborhoods with elevated risk identified by the index are those areas with elevated heat-exacerbated deaths during extreme heat events. HVI scores range from 1 (lowest risk) to 5 (highest risk). Explore the relative heat mortality risk of each Neighborhood Tabulation Area (NTA).
Including race in the HVI analysis is critical to understanding the impact of heat: Structural racism has resulted in neighborhood disinvestment, racist housing policies, fewer job opportunities and lower pay, and limited access to high-quality education and health care, all of which are associated with health risks including those related to heat. Read more about how structural racism affects housing and public health and the history of redlining and how it impacts public health in NYC. The odds of dying are higher in census tracts with higher HVI scores, during extreme heat and on non-extreme hot days.
The best indicator of neighborhood-level heat impacts is the HVI (see map 1), which shows differences in heat-exacerbated mortality risk. The number of heat-stress deaths by NTA (map 2) should be interpreted with caution. The NTAs are small and the number of deaths at this level is also small and unreliable, so it is difficult to tell whether differences between areas are due to random fluctuation or a difference in risk.
Conclusion
Heat contributes to the deaths of more than 500 New Yorkers, on average, each year during the warm season of May through September. In the most recent five-year period (2018-2022) there were an estimated 525 deaths annually. Inequities by race and income persist in the people and neighborhoods most impacted. Deaths across all races, however, were more common at home, underscoring the importance of access to and affordability of home cooling to prevent death.
To prepare for a hotter future and prevent heat-related deaths, the City needs long-lasting, structural interventions alongside heat emergency preparedness and response. Adapting to a hotter climate means the City must:
- Ensure equitable access to life-saving residential cooling for all New Yorkers
- Implement maximum temperature regulations during the summer months for tenants as laid out in 2023 PlaNYC: Getting Sustainability Done.
- Consider mandates on property owners to provide tenants with AC without additional surcharges.
- Help eligible residents apply for a free air conditioner with installation through the Home Energy Assistance Program (HEAP)’s Cooling Assistance Component.
- Protect the electrical grid, which can be strained during hot weather, including by discouraging excess cooling in offices and commercial establishments.
- Work with the State and utilities to make summertime utility costs affordable for low- and middle-income New Yorkers so they can use AC to protect themselves from the heat.
- Make energy prices affordable for all New Yorkers through affordable energy rates for low- and middle-income customers.
- Provide subsidies to help with summer utility costs.
- Prohibit electricity disconnections during hot weather, even if bills are unpaid.
- Fund energy efficient home improvements to help reduce family energy costs and decrease pressure on the electrical grid.
- Invest in local resiliency to make all NYC neighborhoods and residents cooler and safer.
- Implement green infrastructure projects, especially in high HVI neighborhoods, including planting trees and other greenery and expanding cool roofs. For example, expanding the city’s tree canopy coverage to 30% (2023 PlaNYC: Getting Sustainability Done).
- Support community-based organizations (CBOs) working to reduce the health impacts of climate change.
- Include CBOs and residents in decision-making about investments in community infrastructure and public space.
- Fund and provide technical assistance for programs that support CBOs to build community resilience through social cohesion and access to physical and mental health resources that can help people stay safe in the heat.
- Continue to strengthen emergency response to extreme heat, such as opening cooling centers, expanding awareness of other cool indoor spaces, and issuing heat-health warnings, prioritizing people and communities with the greatest need.
- Work with local, state, and federal partners to ensure that indoor and outdoor workplaces are safe during hot weather, such as by setting occupational heat safety standards.
More data and information about heat, climate, and health is available on the NYC Health Department’s Climate and Health page. Learn more about what the City is doing to mitigate the effects of heat as part of PlaNYC: Getting Sustainability Done.
- Bailey ZD, Krieger N, Agénor M, Graves J, Linos N, Bassett MT. Structural racism and health inequities in the USA: evidence and interventions. Lancet. 2017 Apr 8;389(10077):1453-1463. doi: 10.1016/S0140-6736(17)30569-X.
- Vant-Hull, B., Ramamurthy, P., Havlik, B., Jusino, C., Corbin-Mark, C., Schuerman, M., Keefe, J., Drapkin, J. K., & Glenn, A. A. (2018). The Harlem Heat Project: A Unique Media–Community Collaboration to Study Indoor Heat Waves, Bulletin of the American Meteorological Society, 99(12), 2491-2506. Retrieved Jan 30, 2023, from https://journals.ametsoc.org/view/journals/bams/99/12/bams-d-16-0280.1.xml
- Madrigano J, Lane K, Petrovic N, Ahmed M, Blum M, Matte T. Awareness, Risk Perception, and Protective Behaviors for Extreme Heat and Climate Change in New York City. Int J Environ Res Public Health. 2018 Jul 7;15(7):1433. doi: 10.3390/ijerph15071433.https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6069135/
- Metzger KB, Ito K, Matte TD. Summer heat and mortality in New York City: how hot is too hot? Environ Health Perspect. 2010 Jan;118(1):80-6. doi: 10.1289/ehp.0900906. PMID: 20056571; PMCID: PMC2831972. https://ehp.niehs.nih.gov/doi/10.1289/ehp.0900906
- Madrigano J, Ito K, Johnson S, Kinney PL, Matte T. A Case-Only Study of Vulnerability to Heat Wave-Related Mortality in New York City (2000-2011). Environ Health Perspect. 2015 Jul;123(7):672-8. doi: 10.1289/ehp.1408178. Epub 2015 Mar 17. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4492264/